What exactly is gene therapy, and how advanced is Taiwan in the field? Is gene therapy the miracle cure for all disease?
The 21st century, according to some, will be the century of genetic technology. Research is being carried out around the world on the use of genetic techniques against disease, and great hopes are being pinned on the success of this approach.
In the US, gene therapy research has already been under way for seven years, with government funding to the tune of $300 million annually, while the US Department of Health has committed $3 billion to the completion, by the year 2003, of a project to determine the position of every gene in the human genome. In Japan, where "Gene Therapy Year" was held in 1995, gene therapy has been designated a project of national significance.
Gene therapy research in Taiwan began three years ago. Genetic engineering was a focus of interest at last year's fifth National Technology Conference, where it was agreed that "genetic medicine technology" has "considerable implications for national competitiveness," and a cross-departmental program was launched combining the efforts of the National Health Research Institute, the Department of Health, and the National Science Council.
"Genetic research is a global trend, and also the main direction that medicine will take in the future," says Chen Ching-san, biology department director at the National Science Council. Taiwan has to develop the relevant technology if it is not to be left behind.
A far-off dream?
The first "successful" use of gene therapy occurred in 1990, at the US National Health Institute, when it was applied in a case of severe combined immunodeficiency. Yang Wen-kuang, director of the cancer laboratory at the National Health Research Institute and a planner for the Genetic Medicine Technology Program, explains that sufferers from severe combined immunodeficiency disorders lack the genes responsible for producing adenosine deaminase (ADA), an enzyme which is required by lymphocytes in the blood to metabolize adenosine. Without the enzyme, the lymphocytes die off and are unable to provide an immune function. Victims of this type of genetic disorder are susceptible to viral and bacterial infections from the moment they are born, and rarely live beyond the age of three.
The traditional method of treatment involves regular ADA injections to slow the disease. With gene therapy, lymphocytes are extracted from the patient and implanted with the missing gene, before being reintroduced to the patient's body to generate the necessary immunity.
Although that first case made human gene therapy into a reality, a complete cure for such diseases is still in the future. According to Pengwang Chia-kang, director of the Cancer Research Center at Academia Sinica's Institute of Biomedical Science, gene therapy has now been tried in over 200 clinical experiments, and used to treat nearly 1000 patients suffering from a variety of diseases, but a full cure has been achieved for only a handful of those patients. "The first case did not count as a full recovery," says Pengwang, explaining that while the condition of the five-year-old recipient of the treatment improved markedly, the patient, now twelve, still depends on regular ADA injections, as under the traditional method of treatment. The difference is injections are only required every three to six months, rather than every month.
Gene therapy has also yet to realize full cures for hemophilia, cancer and other diseases.
Hsu Ying-chang of Ing Ton Biotechnologies, a company which develops genetically altered animal breeds and carries out cancer research, notes that clinical trials of gene therapy against cystic fibrosis and muscular dystrophy in the US during the past two years have also been unsuccessful.
Genes-the origin of all diseases
Gene therapy has yet to prove itself fully in clinical trials, but the full forces of biomedical research continue to be committed to the cause of this genetic "crusade," now that genes are being linked with more and more diseases.
Lai Chi-ming, director of the cancer wards at National Taiwan University Hospital, who has been treating and researching cancer for over 20 years, says we now know that cancer cells in a tumor are mostly caused by the mutation, loss, transfer and multiplication of genes. "Genes are the 'origin of all diseases,'" notes Lai, "and gene therapy is a way to tackle diseases at their source."
"Gene therapy is definitely the way to go," says Pengwang Chia-kang. The best kind of treatment is specific to the illness being treated, and since we know that so many diseases start with genetic problems, it is natural to focus research and treatment on genes themselves.
So what in fact are genes, and what does gene therapy involve?
Since the mid-20th century, when the structure and genetic function of DNA was discovered, genes have been regarded as the "code" that can unlock the mystery of life, and the "formula" for life itself.
"Every gene carries information about life," says Yang Wen-kuang, explaining that genes are the basic unit of heredity. Every human has 80,000 to 100,000 genes (this has yet to be accurately determined) divided among 23 pairs of chromosomes, and formed of the chemical compound DNA.
"The genes in the human body are like programs on the television," explains Yang. "Some are switched on and some are switched off." For the heart, for example, there may be 30,000 genes "switched on" with the remainder "switched off," whereas a separate 20,000 may be "on" for the stomach. If an individual develops problems with a particular gene that applies to the heart, then any resultant disease will strike at that individual's heart, but have no effect on the stomach.
In simple terms, gene therapy uses techniques from molecular biology to insert healthy genes, directly or indirectly, into human cells, so as to remedy problems caused by defective genes.
There are, broadly speaking, two types of gene therapy. "Gene replacement" involves inserting normal genes into cells, and replacing the original, defective genes by means of DNA recombination. "Gene strengthening," on the other hand, introduces new genes to compensate for the deficiency of weak genes which are unable to perform their normal function.
Curing people, not creating people
The techniques used in gene therapy can also be divided into two types: germ-line therapy and somatic cell therapy. Germ-line gene therapy is carried out, before cell division occurs, on the fertilized cell from which an embryo develops, whereas somatic cell gene therapy involves the direct insertion of healthy genes into cells carrying the source of a genetic disorder.
Professor Wang Tsuo-jen of NTU College of Medicine, elaborates on germ-line therapy: "In theory, the diseases that an individual may fall prey to during his lifetime, can be predicted at the zygote stage of embryonic development. The most effective means of treating genetic disease is to remove the spermatozoon and ovum from the body, and introduce normal genes by micro-injection at the moment of fertilization." The technique has been tried successfully with animals, but there are concerns about applying it to humans.
"How do we ascertain the moment of fertilization?" asks Wang, "and what mutations may result from fertilization occuring outside the body? These issues require great caution." Wang points out that the use of gene therapy on embryos carries wide implications, and that there are ethical, as well as safety concerns, to be addressed. For this reason, notes Wang, somatic cell gene therapy is the more feasible option.
"I too oppose the application of gene therapy at the embryo stage," asserts Yang Wen-kuang. Through experimentation, Yang has found that newborn mice given a genetic vaccination develop lymphatic cancer after five to six months. "Newly born mice are at the same developmental stage as the human fetus in late pregnancy, from which we infer that gene therapy performed during the embryo stage will very likely cause problems for the child later. Caution is essential."
Given the safety, ethical and other considerations, gene therapy on human embryos is still considered "out of bounds." So far, only the somatic cell technique of gene therapy has been applied, and mostly for diseases against which medical technology is otherwise powerless.
As Hsu Ying-chang of Yingteng Biotechnology Co. puts it: "Gene therapy helps God to save people suffering from disease. It is not supposed to replace the hand of God and make flawless humans."
Local crusade
In Taiwan, research into gene therapy is focused on its use for treating cancer.
It is estimated that one in every five deaths in Taiwan can be attributed to cancer, making cancer the island's leading single cause of death since 1982.
According to a report released this year by the World Health Organization, cases of cancer will double in most countries during the next 25 years.
The mortality rate for cancer victims in Taiwan at present is around 75%, far higher than in many advanced nations, such as the US, where the rate is around 48%. Lai Chi-ming notes that there are plenty of factors accounting for Taiwan's high cancer mortality rate. For example, insufficient experience has been accrued in the various applicable methods of treatment, and there is a lack of any overall framework governing medical approaches to the disease. Another important factor concerns the particular types of cancer that are prevalent in Taiwan.
Take the example of liver cancer, which is particularly common among Chinese people. In its early stages the disease often has no symptoms, and it is hard to cure by the time any abnormality is discovered. Liver cancer is consequently considered an especially "malignant" type of cancer.
There are over 200 types of cancer, each with its own characteristics, while congenital and environmental factors mean that the frequency of different types of cancer varies among different races and in different regions.
Yang Wen-kuang says that cancer can have both genetic and environmental causes, but environmental factors-in the form of viruses, chemicals, and diet-predominate. With colon cancer, for example, it is known that at least six or seven types of gene are involved, of which only one type is hereditary. The other genes are mutations associated with the external environment.
Taiwan's Genetic Medicine Technology Project, which brings together experts in biomedicine from their respective national departments, is focused at present on several types of cancer particularly prevalent in Taiwan: nasopharyngeal cancer, liver cancer, cervical cancer and lymphatic cancer.
Yang, who has been involved in cancer research for 30 years in the US, says: "When you encounter a case of nasopharyngeal cancer in the US, you can almost tell with your eyes closed that the patient is Chinese."
"We have to solve our own, localized problems," says Tao Mi-hua, assistant researcher at Academia Sinica's Institute of Biological Research, indicating that it is not practical to wait for the relevant medical technology to be developed elsewhere when a disease has a particularly local prevalence.
"Compound" gene therapy
The traditional methods of treatment for cancer are surgery, radiotherapy and chemotherapy, all of which tackle the manifestation of the disease rather than its root cause.
In recent years, medicine has discovered cancer-causing "oncogenes," as well as other genes which serve to suppress cancer. According to Lai Chi-ming, concurrent damage to two different types of gene is required for cancer to develop, and treatment has to begin with the genes if a cancer is to be cured at its root. The objective is to deactivate the oncogenes and restore the efficacy of the cancer-suppressing genes.
"Gene therapy for cancer differs from gene therapy for hereditary diseases," says Yang Wen-kuang. Hereditary diseases often result from a single defective gene, whereas cancer involves at least five or six types of genes. Since it is not possible to rectify each of the different genes one by one, the only solution is to try and kill off the cancer cells.
Yang has developed a technique called "compound gene therapy" to improve the efficacy of treatment. "It is a similar idea to the 'cocktail' of drugs used in the treatment of AIDS," explains Yang, in that "self-destructing genes" are combined with "immunity genes" to fight the cancer.
Most drugs used against cancer kill off healthy cells as well as the cancer cells they are targeted against, but this problem can be overcome with genes that eliminate themselves. Yang explains that the characteristic of these genes is that they produce a kind of enzyme called protease. When this enzyme encounters a certain kind of drug, which is non-toxic and harmless to healthy cells, it renders that drug toxic so that it kills off the host cell.
Self-destructing genes are not normally present in the human body, but there is such a gene contained in the herpes virus, and it is by means of a virus that the gene can be introduced into cancer cells, where the protease is produced. The patient is then injected with a drug that is non-toxic and harmless to healthy cells, but which becomes toxic on encountering the enzyme in the cancer cells, thereby causing those cells to die.
As researchers have found, cancer does not deprive victims of their immune defenses completely, but rather renders the immune system ineffective by means of immunity-suppressing molecules produced by the cancer cells.
The principle behind "immunity" gene therapy is that the immune system can be regulated and revived using cytokine genes. Genes from hormones are inserted into cancer cells to suppress the growth of those cells, or tumor cells carrying those genes are injected into the patient to generate an immune reaction, thereby suppressing the growth and spread of cancer cells.
Prevention is better than cure
Further to its application as a cure for cancer, gene therapy can also be used to prevent a cancer's recurrence.
Relapse is always a problem in the treatment of cancer. Lai Chi-ming explains that by the time cancer is diagnosed, cancer cells have often spread through the body, and the disease may recur several years later elsewhere in the body, no matter how effective the original surgery was.
Surgery fully cures around one third of colon cancer patients, for example, but the other two thirds suffer some form of relapse. By testing a patient's genes, the spread of cancer cells can be traced, helping doctors to predict where the cancer may recur and enabling them to perform gene vaccination in time.
Gene vaccination, which combines the advantages of both treatment and prevention, is another focus in the development of gene therapy in Taiwan.
Tao Mi-hua, who is actively involved in research in this field, describes gene vaccination as the "third generation" form of vaccine.
By contrast with the first and second generations of vaccine, made from live viruses and viral proteins, the new type of vaccine, which is non-infective, uses DNA to carry one or several varieties of viral gene. The genes are introduced into the body to be absorbed by cancer cells, where they produce antigens and generate the desired immune reaction.
Vaccines to treat and prevent the onset of AIDS have already been introduced overseas, while gene vaccines for use against colon cancer, breast cancer, lung cancer and lymphatic cancer are undergoing clinical trials. In Taiwan, the technique is being studied for the treatment of locally prevalent diseases such as hepatitis B and Japanese encephalitis.
Tao points out that over 90% of Taiwan's population is infected with the hepatitis B virus, and while some develop natural immunity, around 20% of the population, or two to three million people, may be chronic carriers of the disease. These carriers are over 200 times more likely than others to suffer diseases such as liver cirrhosis and liver cancer.
Taiwan is fairly advanced in terms of research into hepatitis B gene vaccination. Tao Mi-hua, who is leading the research, has found, through experiments with rats, rabbits and pigs, that the concentration of antibodies in these animals does increase after injection with the vaccine.
Potential crisis
The prospects look good for gene therapy and gene vaccination, and both should bring great benefits to the human race. At the current stage of development, however, there are problems and side-effects which still need to be overcome.
The biggest hurdle for gene therapy at present is that the right "vector" has yet to be found, enabling safe, accurate and effective delivery of genes to the target cells.
It is viruses that are mostly used as vectors at present. Researchers insert the gene into a virus, which has first been rendered harmless to humans, and the virus is then used to introduce the gene into body cells. Various viruses have so far been tried for this purpose, including retroviruses, glandular viruses, and herpes viruses. Glandular viruses, such as those responsible for the common cold, have proved effective vectors in animal experiments, but far less successful with humans. Yang Wen-kuang explains that since everyone has at some time been infected by and developed immunity against such viruses, their use in small quantities is ineffective for delivery of the required genes. On the other hand, if too much of the virus is used, this may bring on an acute reaction such as asthma.
Unguided missile
Another matter of concern is the possibility of side-effects and complications resulting from gene therapy.
Success in animal experiments is no guarantee that a particular technique is suited for humans. Yang Wen-kuang has observed that rats make a full recovery after somatic cell gene therapy, with no side-effects or complications in either the rats or their offspring. "Rats only live for three years, and can serve as a useful point of reference," says Yang, "but even when no side-effects are observed in rats, the result still has to be confirmed separately for humans."
Using viruses as vectors for the genes is a disturbing risk. "Many viruses are formidable foes," Yang explains, "and even after being broken down they may still re-form or mutate, and revive once inside the body." The possibility of this occuring may be miniscule-perhaps 100 million to one in the past, and 10 trillion to one given recent advances-but it cannot be overlooked.
Another matter for concern is whether or not these viral vectors will penetrate the germ-line cells, where they can be transmitted to and infect the following generation.
Since viruses cannot be tracked within the body, there is no way of predicting where they may end up after killing the cancer cells. This is why gene therapy has been described as both dangerous and unreliable, and likened to firing an "unguided missile."
Pengwang Chia-kang, the earliest proponent of gene therapy in Taiwan, says: "If the virus gets somewhere it shouldn't be, you've got a problem."
Says Yang Wen-kuang: "What worries many people at present is that the virus may enter reproductive cells or an early stage embryo." Once a virus enters these germ-line cells and starts to multiply, it will be present in all the cells of the developing body.
However, notes Yang, there are already several million people in the world with the AIDS virus (a retrovirus) multiplying in their bodies, yet genes for this retrovirus have not yet been found to enter human reproductive cells for transmission to the next generation. This indicates that there is little likelihood of a retrovirus gene vector harming following generations. It is too early to jump to conclusions, however, since retroviruses have so far been used as human gene therapy vectors in only a handful of cases, and they have not yet been under observation for long enough periods.
A further possible outcome of inserting the DNA of a virus into genes within a human cell is that the cell may turn cancerous, or DNA antibodies could be produced which attack the cell itself, causing an auto-immune disease. If the DNA in a cell begins continually producing protein, this too can have negative consequences. In short, the safety of gene-based approaches to treatment has to be very carefully studied.
A risk that has to be taken
It is still early, however, to be worrying about these issues, as gene therapy has a long way to develop yet, proceeding from fundamental experiments, through animal testing to clinical trials. "Let's wait until the technique is able to produce a full cure for something before we worry about the complications," says Pengwang Chia-kang.
"Sometimes it is necessary to take risks with the unknown," adds Pengwang, pointing out that there was at first a great deal of opposition in Taiwan to the introduction of compulsory hepatitis B inoculation for children, on the grounds that it was wrong to subject children to the risk. Ten years later, however, the rate of hepatitis B infection among children has fallen by 70%.
"In my opinion, gene therapy is just like blood transfusion," says Yang Wen-kuang. Blood can also transmit infection and disease, but blood transfusion can still take place, as long as blood that carries pathogens is avoided.
Humans and animals have different genes, and results obtained through animal testing do not necessarily apply to humans. For this reason, clinical trials are an essential stage in the development of gene therapy.
When research into gene therapy began in Taiwan three years ago, it was decided to start with fundamental experimentation rather than proceeding straight to the stage of clinical trials. As Yang Wen-kuang explains: "We cannot rush through this just because others have been through the process already." In contrast to animal testing, the step up to the stage of clinical trials cannot be taken lightly. Only when the fundamental research has been completed and the relevant facilities established, and when gene therapy legislation has been adopted, will the time be right for clinical trials.
During the past three or four months, gene therapy has been used in mainland China for five cases of brain cancer, but it is still too early to know whether the treatment was successful.
"When we start, we must be sure to be better than others," says Yang Wen-kuang. In the US, many researchers in this field began clinical trials, only to find that the problems they encountered had to be solved back at the early stage of research. As a result, there was a return to fundamental experimentation in the US last year.
Certain success
NTU Hospital's GLP (Good Laboratory Practice)-standard laboratory for clinical trials of gene therapy is nearing completion, while the National Medical Research Institute has now drafted the relevant medical code, and it is anticipated that clinical trials can begin as early as the end of the year.
The first such trials in Taiwan will tackle malignant tumors of the brain, as brain cancer is a highly localized disease requiring urgent measures. In other words, the cancer does not tend to spread throughout the body, and must be dealt with quickly if the patient is to have a chance of survival. Li Liang-hsiung, director of neurosurgery at Veterans General Hospital, once said: "In more than twenty years of operations on such patients, only one survived, while the rest succumbed within a year of surgery." As Yang explains, most victims of malignant brain tumor suffer a relapse within three months of the operation.
According to Pengwang Chia-kang, "people shouldn't hope for too much from gene therapy." Although it is a promising method of treatment, there is still much work to be done and many difficulties to overcome, and we should not start hoping for miracles.
Medical technology has always been driven to challenge disease, and the gene crusade is no exception. For the outcome, we must wait and see.
p.106
Humans normally have 23 pairs of chromosomes. (drawing by Liao Tzu-wen)
p.107
A chromosome (top) and the double helix of DNA (bottom) from which it is formed. DNA is the main constituent of heredity. Genes are segments of DNA, and there are thousands of genes arranged on the DNA of every chromosome.
p.109
Cancer has been Taiwan's leading cause of death for the past 15 years. High hopes are pinned on research into gene therapy. (photo by Hsueh Chi-kuang)
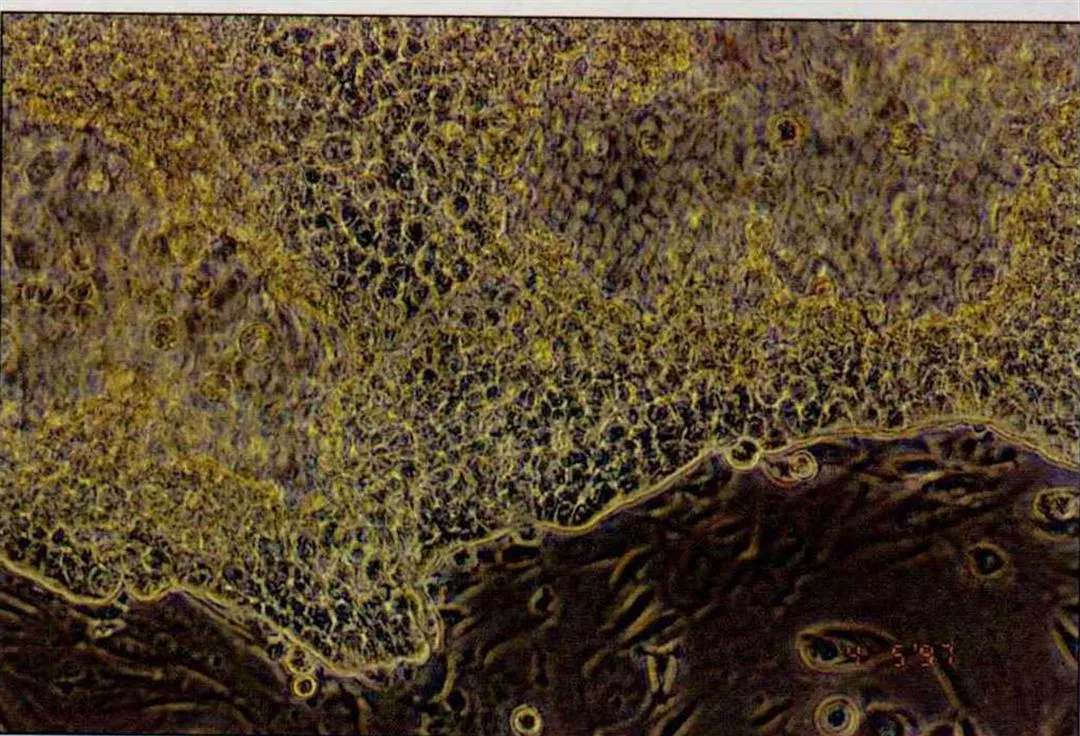
Cancer results from certain changes in the genes. In the top picture, closely packed cancer cells can be seen in the process of multiplication. Normal cells, more widely spaced, are shown below. (courtesy of Yang Wen-kuang)
p.111
How gene therapy works.
Gene
Virus
1.A gene capable of making the patient's missing enzyme is inserted into a virus.
2.Long-lived stem cells, which produce immune cells, are flushed from the patient's bone-marrow into the bloodstream, and then extracted.
3.The stem cells are mixed with the genetically engineered viruses, enabling the viruses bearing the new gene to enter the stem cells. With this gene, the stem cells are now able to make the missing enzyme.
4.The stem cells are injected back into the patient, in the hope that they can permanently strengthen the immune system.
courtesy of Pengwang Chia-kang
drawing by Liao Tzu-wen
p.112
Browning of the cells shows that the genes have entered and begun to take effect. (photo courtesy of Yang Wen-kuang)
p.113
Gene therapy research in Taiwan, focused mainly on cancer treatment, is still at the experimental stage. (photo by Vincent Chang)
p.114
Experimental immunization of a laboratory mouse.
Irradiated tumor cells are injected into the mouse to generate immunity.
Living cells from the same tumor as the original irradiated cells are injected.Living cells from another tumor of the same type are injected.
Living cells from an unrelated tumor of a different cell type are injected.
Tumor cells are eliminated by the immune system.
Tumor cells are eliminated by the immune system.
Tumor cells are not eliminated, and the tumor grows.
courtesy of Pengwang Chia-kang
drawing by Liao Tzu-wen
Cancer has been Taiwan's leading cause of death for the past 15 years. High hopes are pinned on research into gene therapy. (photo by Hsueh Chi-kuang)
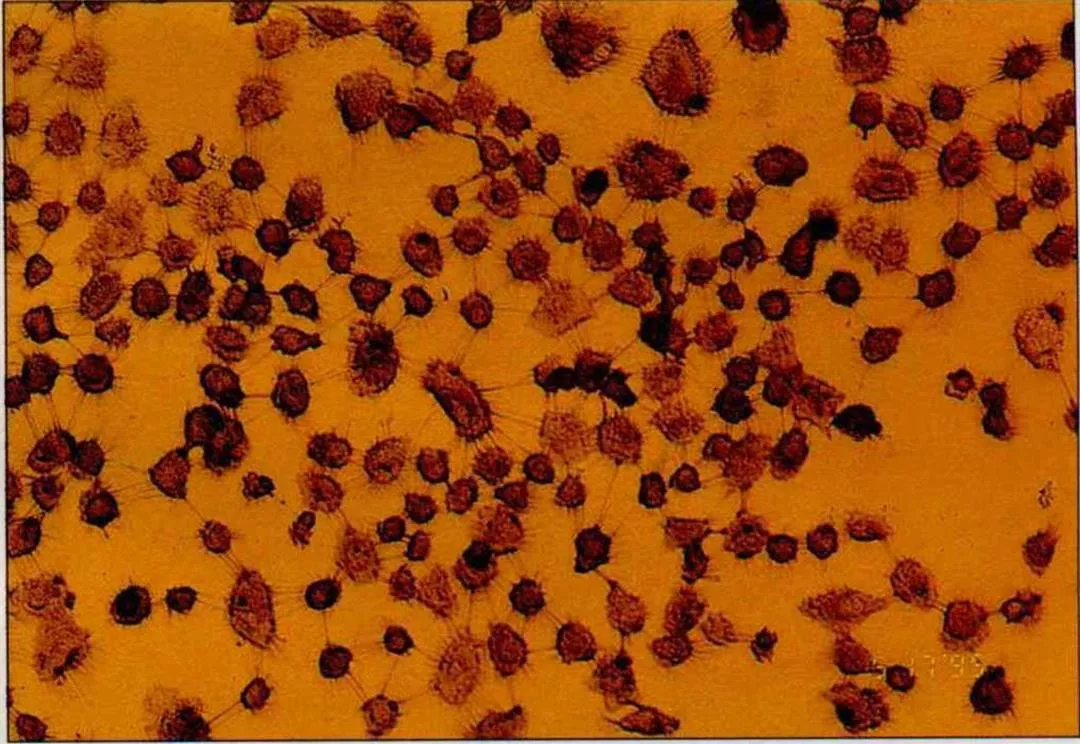
Browning of the cells shows that the genes have entered and begun to take effect. (photo courtesy of Yang Wen-kuang)
Gene therapy research in Taiwan, focused mainly on cancer treatment, is still at the experimental stage. (photo by Vincent Chang)