Alarm Bells in Children's Healthcare
Chang Chiung-fang / photos Hsueh Chi-kuang / tr. by Paul Frank
June 2007

"Taiwan doesn't value children's healthcare," laments Dr. Huang Fu-yuan, senior pediatrician and vice superintendent of Mackay Memorial Hospital. Difficult though it may be to believe, Dr. Huang warns that pediatric medicine faces an unprecedented crisis in Taiwan.
At a time when there is no policy on the horizon to stem Taiwan's rapidly falling birthrate and every child is a supposed to be a treasure, can it really be true that we don't value our children? What kind of crisis is pediatric medicine facing?
On the whole, great strides have been made in children's health in Taiwan.
Lin Tzou-yien, president of the Taiwan Pediatric Association and director of Chang Gung Children's Hospital, notes that advances in public health and the development of new vaccines have resulted in a sharp decline in infectious diseases. In addition, prenatal healthcare efforts have effectively prevented the spread of many hereditary diseases. For example, thalassemia has become much rarer among Taiwanese children.
According to Lu Hung-chi, professor emeritus of pediatrics at National Taiwan University Hospital and director of St. Mary's Hospital Lotung, pediatric health studies conducted over the past 40 years indicate that from 1965 to 1985, Taiwan's infant mortality rate (IMR) from birth to one year of age fell from 24 per 1000 births to seven per 1000, and from ages one to four years it fell from 4.7 per 1000 to 0.9 per 1000. This was remarkable progress, but Taiwan's infant mortality rate has stagnated since 1985, and remains twice as high as those of advanced nations such as Japan, Singapore, and Sweden.
Recent Department of Health statistics indicate that Taiwan's IMR for children below age five stands at 7.82 per 1000 (in 2004), and remains somewhat higher than in Singapore (3), Japan (4), South Korea (5), and Sweden (5).
What accounts for this bottleneck in children's healthcare in Taiwan? Lu Hung-chi thinks that a rise in accidental injuries (such as traffic accidents, falls, and drowning), insufficient early detection of childhood diseases, and a failure to treat serious illnesses as effectively as a number of advanced countries have contributed to Taiwan's stagnating IMR.
Lu notes that 20% of cases of congenital heart disease are not detected in preschool children, and are only found during health check ups when the children start school.
Taiwan also lags behind in the treatment of serious childhood illnesses. For example, childhood leukemia typically has a good prognosis, but in Taiwan the cure rate for this disease is 40-70%, compared to 80-90% in advanced countries.

Accessibility is a major strong point of children's healthcare in Taiwan. Because children have immature immune systems and are highly susceptible to respiratory infections, their parents frequently take them to clinics for treatment.
Indicators of progress
Children are an important national asset and children's healthcare is also regarded as an indicator of a country's level of modernization. In Taiwan, healthcare is currently beset by a number of systemic and structural problems awaiting solution.
"Taiwan lacks a national-level children's hospital," says Lin Kai-hsin, a pediatric hematologist-oncologist who directs the Preparatory Office of National Taiwan University Children's Hospital. In the advanced countries of Europe, North America, and Japan, on the other hand, almost every big city has a specialized pediatric hospital.
Most people may wonder why children's hospitals are necessary. What's the difference between a children's hospital and a pediatric department in an ordinary hospital?
"A specialized children's hospital provides integrated care," explains Dr. Lin. Unlike general hospitals, where the focus is on adults, children's hospitals naturally put children first and provide care from the mother's womb, including prenatal genetic health counseling, to adulthood. Their departments of obstetrics, genetic medicine, pediatrics, ophthalmology, dentistry, and plastic surgery enable such hospitals to offer a full range of pediatric services.
Chang Gung Children's Hospital is currently Taiwan's only exclusively pediatric hospital in name and practice. Located in Linkou, Taoyuan County, the 500-bed hospital has an intensive-care unit with more than 100 beds, which makes it second only to Beijing's and Toronto's children's hospitals.
Nonetheless, as a private hospital that faces enormous pressures and cannot afford to operate at a loss, Chang Gung Children's Hospital sometimes diverts empty beds to adult patients. Moreover, for critical medical care that places a heavy burden on manpower and material resources it still depends on help from national-level public hospitals. As early as 1984, plans began to be made for National Taiwan University Children's Hospital, which is slated to be a national-level hospital. Construction of its high-rise building is more or less completed and it is expected to open in 2008. The hospital will specialize in pediatric critical care medicine.
Lin Kai-hsin points out that although the goal of National Taiwan University Children's Hospital is not to make money, its planning process has not been smooth sailing, and given that pediatric critical care medicine is very costly, it is difficult to predict whether it will incur losses no one will be willing to shoulder.

Thalassemia major often requires lifelong blood transfusions. In addition to increased prenatal screening, doctors also perform bone marrow and umbilical cord blood transplants to alleviate the symptoms and bring this disease under control.
More bang for your buck
Although much remains to be done to improve pediatric critical care medicine, there is no denying that in terms of accessibility, Taiwan's primary care system is very good indeed. Few other countries can match Taiwan's primary care services. Within the framework of the National Health Insurance (NHI) system, there are currently 18,877 clinics, including 2-3,000 small and medium-sized clinics specializing in pediatric and family services.
Moreover, Taiwan boasts a unique combination of low consultation and treatment fees and easy access to doctors in teaching hospitals. Huang Fu-yuan notes that in Taiwan a single deductible outpatient consultation fee comes to between NT$50 and NT$360, compared to more than NT$1,000 in Japan and more than NT$2,000 in the USA. Taiwanese patients get more bang for their buck.
Children's healthcare in Taiwan is easily accessible and low priced, but there is a lack of comprehensive care and a tendency not to see the forest for the trees. Parents often have to hunt far and wide to find a doctor for their child. Examples of wasted medical resources, misdiagnoses, and delayed treatments can be found everywhere.
A six-year-old child who was occasionally coughing up blood was taken to three clinics, all of which failed to find out what had caused the problem in the first place. The first doctor diagnosed TB, the second concluded it was gastroenteritis, and the third thought that allergic asthma was the cause. Hearing three different diagnoses from three different doctors only confused the parents and made them doubt all three doctors. In the end, they went to Huang Fu-yuan at Mackay Memorial Hospital. Dr. Huang did not even have to conduct a close examination; he simply asked the parents whether the blood-coughing episodes had been preceded by nose bleeding, and when they said yes, he determined that the child had simply coughed up blood that had flowed back down the throat.
"In 20% of pediatric outpatient consultations, children don't require any treatment. What they need is a patient and experienced doctor to set the parents' minds at ease," says Huang Fu-yuan.
Another child who had been diagnosed with gastroenteritis following a recent history of vomiting was taken to Huang's clinic. The child had been examined three times in a clinic and had also been prescribed medicine, but the symptoms had not disappeared. In response to detailed questioning by Huang, the mother mentioned that in addition to vomiting, her son walked unsteadily. Vomiting and an unsteady gait are typical symptoms of a tumor. Huang's experience immediately made him suspect a brain tumor, and a subsequent test confirmed his fear.
As can be seen from these examples, it is difficult for a doctor to make an accurate diagnosis when examining a child who is unable to give an accurate description of his or her symptoms. Looking no further than the obvious symptoms makes it difficult to avoid misdiagnoses.
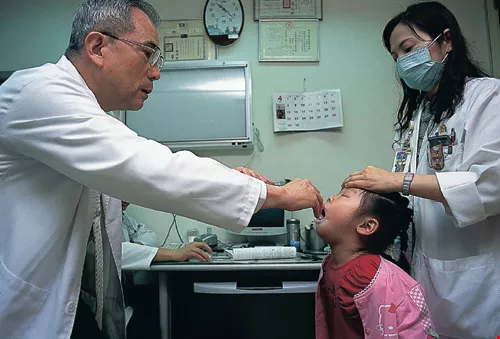
Diagnosing children is difficult and time consuming. The photo shows Dr. Huang Fu-yuan of Mackay Memorial Hospital at work.
Can every doctor treat children?
The fact is pediatrics is a specialized field of medicine. It is certainly not the case that every doctor can treat children, but Taiwan's public is insufficiently aware of this.
"Children are not miniature adults," notes Huang Fu-yuan. Children's physiological markers and disease symptoms are different from those of adults and should on no account be lumped together with theirs.
The childhood years before the age of 18 are a period of continuous growth and development. Because children's organs and body systems mature with each passing day, at different ages their anatomy, heart rate, blood pressure, and respiratory rate are different (the heart and respiratory rates slow down with age, whereas the blood pressure rises). For example, a newborn takes short and rapid breaths--about 40 per minute--but by the time the child is 18, the rate has gradually slowed down to about 18 breaths per minute.
Common childhood illnesses are not the same as the illnesses commonly seen in adults. Because their immune system is immature, children's ability to resist infections is limited and they are quite susceptible to "minor" respiratory and digestive tract diseases.
Huang Fu-yuan notes that the most common early childhood diseases, accounting for 30-40% of the total, are upper respiratory infections, pneumonia, and bronchitis; the second most common is acute gastroenteritis, accounting for 20%; and the third are urinary tract and kidney diseases. As a result of environmental and dietary changes, in recent years Taiwan has experienced a rising trend in childhood allergies and metabolic disorders (such as diabetes), as well as childhood obesity.

If a child who is forced to wear adult shoes has difficulty in walking, what about a child who is forced to use a wheelchair designed for adults? Most of the equipment and concepts used in Taiwanese children's healthcare were originally developed for adults rather than children.
Not miniature adults
Not only are common childhood illnesses different from common adult illnesses, but even the same illness exhibits different symptoms and courses in children and adults.
Urinary tract infections are common in diaper-age children. But whereas in adults the typical symptoms (painful, urgent, and frequent urination) make it easy to diagnose such infections, in infants and toddlers the typical symptoms (fever, irritability, vomiting, and diarrhea) appear to be completely unrelated to the urinary organs. If the physician is not alert to this, he can easily mistake a urinary tract infection for a common cold or gastroenteritis.
Myocarditis, a condition that is often seen in children and can easily result in medical malpractice disputes, is also difficult to diagnose. Huang Fu-yuan explains that one of the early symptoms of myocarditis is fever, which is also typically associated with the common cold. A general practitioner who neglects to listen carefully to the child's heart while conducting the diagnostic examination can easily miss this disorder. Unfortunately, because myocarditis is a rapidly progressive condition, even a small delay in treatment can easily prove fatal.
In other countries, it is a matter of course that a child who falls ill is taken to see a pediatrician. In Italy the law requires that children under six be treated by pediatric specialists. But in Taiwan, it is commonly believed that anyone who has a medical license is a doctor and that's that; in other words, it is assumed that not just pediatricians, but ear, nose and throat (ENT) specialists, family practitioners, gastroenterologists, and dermatologists are all qualified to treat children.
According to Taiwan Pediatric Association statistics, approximately 40% of Taiwanese children under three have seen a pediatrician, 30% an ENT specialist, and 20% a family practitioner.
The "chaotic state" of front-line medical practice greatly increases the risks of children's healthcare. "ENT specialists can only examine and treat part of a patient's body. Because they rarely examine a child from head to toe, they cannot identify and diagnose problems outside their field of expertise. Family practitioners receive only three short months of pediatric training in medical school and may never even have come across a serious childhood illness such as an enterovirus infection. How can they be expected to make correct diagnoses?" asks Huang Fu-yuan.
"The more you see, the scarier it gets," says Lin Tzou-yien. Children are full of vitality and have a fast metabolism, but they often get violently sick and when they do, the illness can progress so quickly that it has to be monitored from hour to hour. Reye's syndrome (a form of encephalitis of uncertain cause which usually occurs after viral infections) often deteriorates to a coma within a few hours of onset. There have also been many cases of severe enterovirus infections that resulted in death within 24 hours of hospitalization. The initial symptom of meningitis is a temperature very much like that associated with a cold, but within one or two days the patient's condition can take a dramatic turn for the worse. Many parents who lose a child accuse the doctor of misdiagnosis because they don't understand that it is quite possible for a child to be playing happily one minute and fall ill beyond recovery an hour later.
You get what you pay for
"During each stage of their children's development--which happens very fast--it is very important for parents to have them vaccinated, give them proper nutrition, and educate themselves about the growing process," says Lin Tzou-yien. He stresses that only when the prevention and treatment of childhood diseases is integrated and pediatricians do timely public health education work will comprehensive children's healthcare be achieved.
So much for the ideal, but "the biggest obstacle is a lack of resources," says Huang Fu-yuan, hitting the nail on the head. Huang points out that children's hospitals in Europe and North America can count not just on income from insurance companies but also on very generous donations. Big-name movie and sports stars organize benefits to raise money for children's hospitals, while visiting royalty and heads of state are sure to be taken to see them. In Japan, insurance companies pay hospitals 26-48% more to treat a child than they do for an adult undergoing the same treatment. By comparison, children's healthcare gets short shrift in Taiwan. Particularly since the "global budget" system (in which hospitals receive lump sums from the NHI program to cover their medical expenses for each fiscal year) was introduced in 2002, children's healthcare has been squeezed for funds.
Because children tend to cry and are difficult to control and communicate with, providing outpatient pediatric services is more demanding and requires a higher investment in time and personnel. For example, an electrocardiogram or an echocardiography can be performed in ten minutes on an adult, but it may take more than 40 or 50 minutes in the case of a child. Such problems result in higher costs that are not reflected in the payments received for the treatment.
Huang Fu-yuan notes that children under 18 comprise 26.7% of Taiwan's total population but only 12.5% of NIH payments, which is less than is spent on dialysis. On the other hand, the 9% of people who comprise the elderly population use up 33% of NHI payments. "More than half of healthcare expenditures are made in the six months prior to death," says Lin Tzou-yien, who asks whether a under a system and mindset that "cares more for the dying than the living" the masters of the nation's future are receiving woefully inadequate medical care.
The last straw?
A new NHI payment system will be introduced in January 2008 which will put patients into diagnosis-related groups (DRG) irrespective of individual differences. For many financially strapped hospital pediatrics departments, this may well turn out to be the straw that breaks the camel's back.
Pediatric medicine has always been a drain on personnel and financial resources. Many big hospitals are unwilling to invest in pediatric departments and even university medical centers do not necessarily have a full range of pediatric equipment. It is no more reasonable to ask a toddler to wear adult shoes than to force children to share X-ray and electrocardiogram machines with adults, but that is precisely what is happening. Doctors who have to deal with life-and-death situations can only stomp their feet in frustration.
"Even the country that spawned the ill-advised DRG system--America--does not include children's healthcare in it," says Lin Tzou-yien bluntly, adding that this kind of system can create a situation of "selective healthcare." In the future, warns Lin, cases such as that of "Little Sister Chiu" (a four-year-old girl who died after being turned away by several hospitals following a severe beating by her alcoholic father) will occur again and again in Taiwan. This is particularly true in the case of critical-care medicine that involves high human and material costs and long-term care. For example, there will not only be a lack of money and doctors to treat major childhood diseases, congenital anomalies, and septicemia, but even research and teaching in these areas will take a big hit.
Besides the fact that when the NHI system was introduced, no thought was given to the special characteristics and problems of children's healthcare--an omission that has resulted in underfunding in pediatric care--in recent years Taiwan's birthrate has registered a rapid decline. Last year, for the first time, the number of births fell below 200,000. The children's healthcare market is shrinking and pediatricians are grumbling. The number of primary pediatric clinics has fallen from more than 100 during their heyday a decade ago to fewer than 30 today. Even in big hospitals, pediatricians have had to accept salary cuts. As hospitals have come to consider pediatric care a losing proposition, pediatricians have become second-class citizens in the medical community.
Fewer choose pediatrics
"The fuse is burning short," says Huang Fu-yuan, and no one in pediatrics knows where the money is going to come from. The Department of Health approved an upper limit of 240 new pediatric residents this year, but so far fewer than 100 have been recruited. Each hospital can only afford to recruit 40% of the pediatric residents it needs and has to make up for the staff shortage with nurses. Lin Kai-hsin feels very strongly about this. He says that most pediatric residents choose less demanding specialties. It has been several years since anyone specializing in his own field of pediatric hematological oncology (leukemia) was hired.
Because children's diseases are highly volatile and frequently lead to malpractice disputes, pediatricians are always watchful of possible pitfalls and fearful of making mistakes. They also face enormous pressure from unreasonable parents who demand that they immediately bring down their child's temperature, call them at the slightest hint of illness, and insist that they be on call at any hour, never allowing them a moment's rest. For these reasons, many newly graduated pediatricians throw in the towel after six months and change to a less demanding specialty.
The market is shrinking and pressure is growing. The fact that fewer and fewer medical students are choosing pediatrics as their specialty seriously threatens the future quality of pediatric medicine in Taiwan. "Unless we figure out a way to remedy this situation, we risk destroying the foundations of our country," warns Lin Tzou-yien.
Children are the adults of the future. A healthy citizenry tomorrow depends on healthy children today. Children are full of vitality and have a remarkable capacity to recover quickly from most illnesses, but although pediatric medicine is demanding and costly, no matter how we figure it, offering children good healthcare wherever they live is an investment the nation and society cannot afford not to make.


@List.jpg?w=522&h=410&mode=crop&format=webp&quality=80)



