Rebuilding the Missing Link--Toward the Rebirth of Taiwan's Public Health System
Teng Sue-feng / photos Yang Chien / tr. by Anthony W. Sariti
August 2003

The outbreak of an epidemic of the pre-viously unknown disease SARS (severe acute respiratory syndrome) revealed a Taiwan public health system shot through with flaws. But twenty years ago, Taiwan had suppressed malaria, Japanese encephalitis, infantile paralysis, and other infectious diseases and had successfully set up a powerful frontline, grassroots defense network against epidemics. Why wasn't Taiwan been able to continue that tradition and capitalize on that experience? How can the cracks in the current system of epidemic prevention be repaired?
At the end of April in-hospital infections broke out in Taipei's Hoping Municipal Hospital and Jenchi Hospital. After some residences in the Huachang Public Housing Complex on Tali Street were quarantined, the Wanhua District became the center of the epidemic.
From morning till night, the phone at the Wanhua District Health Center rang off the hook. Because many people with chronic illnesses were afraid to go to hospitals, "the responsibility for people quarantined at home and for those with chronic illnesses all fell to the public health center," says Head Nurse Chen Ching-chu from the Wanhua District Health Center. The work just came flooding in: from sending out quarantine notices, delivering food, and helping with temperature taking in veterans homes, to assisting kidney dialysis patients find hospitals to go to and giving medicine to the chronically ill. An estimated 200 public health workers from Taipei's twelve administrative districts were faced with over two million nervous city inhabitants. The enormous workload that materialized in short order was truly exhausting.
"We were all running temperatures, but it wasn't because of SARS-we were completely exhausted," says Chen Ching-chu. The Taipei Department of Health knew there were not enough first-line personnel and sent people from the Department of Civil Affairs and the Department of Social Welfare to help. Additionally, there were volunteers who threw themselves enthusiastically into the work. Nevertheless, many were unfamiliar with the complex pattern of small streets and alleyways of the Wanhua District. They had to be accompanied by Heath Center personnel even when delivering meals and were unable to be of immediate help.

During hot summer days, one must be careful to guard against the spread of intestinal viruses and dengue fever. Establishing good personal hygiene habits starts with careful hand-washing. (photo by Hsueh Chi-kuang)
A history of disease
Public health workers, originally at the frontline of community epidemic prevention, ended up performing menial tasks like delivering lunches and emptying garbage cans. For many people, this was an incredible turn of events. A glance at the history of Taiwan's public health system showed these workers, deployed at the grassroots level, had a vast reservoir of personal experience and had constituted the primary force in fighting epidemics. Taiwan, situated in the Asian tropical zone, had historically been seen as a breeding ground for pestilence. The Han people who braved the trans-strait voyage from China to Taiwan in early times had to face a struggle against disease and pestilence after their arrival. Less than one out of ten was able to survive the three-fold test of the voyage, the natives and the diseases.
Qing Dynasty officials regarded Taiwan as dangerous, frequently remarking it was like traveling to a "faraway poisonous swamp" and "putting one's life into the hands of the gods." Several officials who came to Taiwan on imperial inspections, like Fukien Inspectors Wang Kai-tai, Ding Ri-chang and Wu Zan-cheng, contracted diseases and died soon after returning to the mainland. Japanese scholars have determined that the death at age 39 of Zheng Chenggong (1624-1662), the Ming dynasty loyalist who expelled the Dutch from Taiwan, was probably from a fever.
During the occupation of Taiwan, the Japanese began to improve public health, the primary reason being that although the Japanese had been victorious, more troops had died of disease than battle. In the battle of Mutan only some 600 men were killed in combat, while over four thousand died of disease. To ensure the safety of those sent overseas and stabilize control of the colony, the Japanese government began to improve Taiwan's health system after the war. They set up medical institutes, trained medical personnel, created an administrative apparatus for public health, determined categories of "legally recognized diseases" (instances of which had, by law, to be reported to the government), issued regulations for shipboard health inspections and set up infectious disease hospitals and malaria prevention centers. In environmental hygiene, the Japanese employed an Englishman as an advisor and planned drainage systems to run above and below ground.
The most successful anti-epidemic measure dating from the occupation period was aimed at bubonic plague, which was eliminated on Taiwan by 1918.
After World War II, work on epidemic prevention in Taiwan was directed by the Nationalist government and the United States. The Nationalist government took over from the Japanese the hospitals and basic level public health services. It also began to set up its own health centers in rural townships, while in villages in more remote areas and mountains it set up health offices that were locally responsible for such things as diagnosis and treatment, control of infectious diseases, mother-child health, hygiene education, environmental and school hygiene, etc. The government thus set up a pyramid-shaped public health system. In 1954 there were 360 health centers in Taiwan and 140 health offices. In the more than twenty years from 1947 to 1970 victims of "legally recognized diseases" dropped from nearly 6000 per year to just over 300.

Although the SARS epidemic is under control, densely populated cities and serious air pollution mean that new infectious diseases could flare up whenever the opportunity presents itself.
All "enemies" destroyed?
Before the takeoff of the economy, when material conditions were still anything but comfortable, Taiwan struggled with many infectious diseases. But during this era the country depended on the doctors, midwives, nurses, and house-call personnel of the health centers who worked with the precinct captain under the residency administration system going door to door inspecting for epidemics and conducting hygiene education. Examples were inoculating infants with vaccines, spraying DDT in neighborhoods, and inspecting pupils in schools for parasites. As a result, by the 1980s Taiwan had successfully suppressed a great number of health-threatening infectious diseases, including malaria, tuberculosis, and infantile paralysis.
The odd thing is that precisely because Taiwan's public health system was so successful in the past-because the "enemy" had been defeated in every battle-people became inattentive to public health. As time went on, frontline public health personnel neglected their training and lost completely their fighting edge. The long string of historical successes won by Taiwan's public health system abruptly came to an end.
Chen Meei-shia, director of the Department of Public Health at National Cheng Kung University, points out that in the 1980s the government's policy of "emphasizing disease prevention over disease treatment" took an about-turn when it began to assist and encourage local health centers to transform themselves into treatment centers, with the result that the health centers changed from entities responsible for public health policy into agencies offering clinical services on a for-profit basis.
A doctor from a health center located in a southern county, who wishes to remain anonymous, says that when SARS hit, because the center had been converted into a treatment center, more than half their time was spent in examining patients rather than doing general epidemic prevention work. Indeed, even now the government lacks a clear focus for future tasks such as promoting cervical examinations, encouraging neighborhood environmental hygiene, or taking preventive measures against chronic diseases.
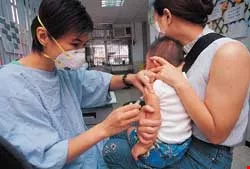
The function of the grass-roots level health office is not limited to administering inoculations. When an epidemic is spreading, health office personnel must shoulder the responsibility for the health of those quarantined at home and for working with the civil authorities and environmental agencies to combat the disease.
No ease for disease
The turnabout in Taiwan's public health policy in the last 20 years has led to a very unbalanced allocation of resources. As resources for treatment have steadily risen, those for public health have seen no corresponding increase at all. In 1986 Taiwan's entire public health force numbered about 3800 people, while those working in the treatment sector numbered some 70,000. By 2001 treatment sector personnel had more than doubled, ballooning to 160,000 people-all this while public health personnel had only increased by 48% for a total of 5700 people.
As Chen Meei-shia describes it, the resources for public health and for treatment are like a dwarf and a giant respectively. "As the population grew, the government steadily encouraged and supported the building of treatment institutions," she says. "As a result, a great deal of capital flowed into the health treatment industry." She points out that these new treatment facilities are, for the most part, owned by syndicates or private individuals whose first consideration is that the hospitals they run make a profit.
According to Department of Public Health statistics on national health expenditures, in 2000 there was an investment of NT$500 billion but only NT$18.2 billion of that (3.3%) was used for disease prevention, public health education and public health services.
The public health system lacks resources, and its effectiveness declines day by day, yet diseases never rest. Changes in the global environment, such as the rise in global temperature, the increase in urbanization, population density, air and water pollution, overuse of antibiotics, etc., have led to a continuing deterioration of the environment so that epidemic diseases that were successfully suppressed some time ago are now fighting back, and bacteria and viruses are more difficult to wipe out.
In March of this year, a rare case of adult Japanese encephalitis was contracted in Kaohsiung. The victim was a 21-year-old student. Japanese encephalitis is primarily transmitted by the bite of the culex tritaeniorhynchus mosquito. For many years the infection rate of this disease has been dropping due to a comprehensive program of childhood inoculation. The appearance now of the adult form of the disease may be related to an incomplete inoculation program or a diminution of antibodies in the blood of the population.

Before the take-off of the Taiwan economy, UNICEF set up "milk stations" in rural areas as a supplement for child nutrition. (photo courtesy of DOH)
When the going gets tough....
On the one hand, the grassroots public health system is powerless to take on the responsibility for disease prevention because of its weakened condition; on the other hand, the treatment sector has developed into an immense structure no one can control. The current epidemic prevention campaign has led even the president of National Taiwan University Hospital and local public health departments to issue complaints that "the Department of Health is unable to control the syndicate hospitals" and that "SARS victims have all been pawned off on public hospitals." The high degree of privatization of hospitals has certainly created some obstacles for disease prevention.
The result of making health treatment a market commodity is that preventative medicine, which makes no money, is not highly regarded. For example, equipment for negative-pressure sickrooms for infectious patients is very expensive yet only a few patients can be accommodated at a time. Some hospitals simply don't set up negative-pressure sickrooms. For the same reason, there are not enough doctors in infectious diseases departments. There are only 200 epidemiologists nationwide. At National Taiwan University Hospital (NTUH), for example, there are only 17 doctors in the infectious diseases department; there is simply no comparison with the internal medicine department with its more than 200 doctors. At Hoping Hospital there are only three epidemiologists. One of the reasons for this is that the doctors in the infectious diseases department are part of the specialty where "you train troops for a thousand days then use them at a single stroke" (when an epidemic breaks out).
If the preventative medicine link in disease treatment and diagnosis is missing, then, faced with a new infectious disease, the medical community is pretty much at a loss about what to do. This also leads doctors indiscriminately to prescribe antibiotics rather than try to discover the actual cause of the disease. Chen Chien-jen, newly appointed minister of the Department of Health, says that tuberculosis, which had all but disappeared from the scene in Taiwan, has once again become an epidemic crisis because of the increase in strains of drug-resistant varieties of the disease. In 2001 there were 1299 deaths attributed to TB, with half that number resulting from these drug-resistant strains.
"Currently there are very few students who have received specialized training in epidemiology," says Professor King Chwan-chuen of the Graduate Institute of Epidemiology at National Taiwan University. "Were an infection to break out in a hospital, none of them would have any idea of where the 'common source outbreak' originated." To avoid infections, hospital planners must give thought to areas such as building design, ventilation, work safety, environmental hygiene, fluid mechanics, communicable diseases, hospital management, mental health, and hygiene education. Because many hospitals had paid little heed to epidemiology, they were forced to stand helplessly by, able only to be reactive and seek outside assistance once they discovered the SARS infection had begun to spread.

In the early years, many children suffered from the disease of internal parasites. Medical personnel regularly visited primary schools to conduct anal exams, collect stool samples and administer medicine-with excellent results. (photo courtesy of DOH)
Helpless in the face of old diseases
The decline in the grassroots public health system not only meant helplessness in the face of a new epidemic, what was worse, when a once-preventable infectious disease flared up anew, it was difficult to suppress. A perfect example of this is dengue fever.
Dengue fever is popularly known in Taiwan as "Heavenly Dog Fever." It is an acute infectious disease caused by a virus infection transmitted by the Aedes aegypti ( L.) and the Aedes albopictus (Skuse) mosquitoes. Symptoms of the disease are high fever, severe headache, muscle and joint pain, nausea, vomiting and skin eruptions. During fever there can be bleeding from the gums and nose which, if serious, can lead to shock and death.
The earliest record of dengue fever in Taiwan dates from 1870. In 1942 some five million people, representing 83% of the total population of the time, were infected by a dengue epidemic. After a forty-year hiatus, in 1981 dengue fever broke out anew in Liuchiu Rural Township, Pingtung County. About 8000 people were infected, some 80% of the rural township's overall population.
According to the Department of Health's Center for Disease Control, studies have shown that the reason for the outbreak of dengue fever in Liuchiu was that there had been no instances of the disease in 40 years and consequently few people had adequate antibodies against it. So when local fishermen landed on the shores of Southeast Asian countries, contracted the disease and then brought the virus back to Taiwan, it was spread by local carrier mosquitoes, leading to an outbreak that soon got out of control. Making matters worse, health workers had long since lost their sense of fear and had become lax. In the end, this all led to a tragedy where almost the entire township "went under."
Until 1994 dengue fever had only occurred on a large scale in southern Taiwan. The central and northern part of the island had not been threatened. But in 1995 a case suddenly did crop up in Taipei County that drew serious attention from the Department of Health because it suggested that the disease was moving north. As a result, over the last few years as Taiwan enters each summer season, everyone is on full alert.
When dengue fever was attacking southern Taiwan, the average health center in a rural township had only five employees. But communities there are spread widely and it required a great deal of time and personnel to visit each and every community and inspect outdoor containers of standing water, destroy carrier mosquitoes, and spray disinfectant. A doctor from a southern county admits that dengue prevention work had not been very good.
New wine in an old bottle
The fact that a disease previously wiped out is now difficult to control shows the epidemic prevention system does indeed leave a lot to be desired. Where should this work of putting "new wine in an old bottle" begin?
Chen Meei-shia, director of the Department of Public Health at National Cheng Kung University, emphasizes that, compared with today, before 1970, when economic conditions were not as good as they are now, the government was really only able to provide the public health system with meager resources. Despite this, good work was done because the national policy was very clear, as indicated by their motto: "public health [i.e., prevention] is more important than treatment." Thus, public health circles have high expectations resulting from the appointment of Chen Chien-jen as minister of health, since he comes from an epidemiological background and his appointment reversed the usual practice of appointing a minister of health from the treatment sector.
In June, as the SARS epidemic abated somewhat, Taipei City Councilor Hsu Chia-ching organized a symposium on "Community Epidemic Prevention and Public Health" to which she invited the superintendents of Taipei's municipal hospitals as well as grassroots health center personnel to voice their opinions.
"You really have to feel sorry for our nursing staff," says Head Nurse Chen Li-hua of Hoping Hospital. It fell upon her to speak for health care workers at the grassroots. The average district in Taipei City has a population of more than 200,000, but on average there are only seven public health nurses per health center . . . how can they cope? Also, Hoping Hospital originally had more than 400 nurses, yet when the hospital was cutting personnel costs it made certain to first cut the nursing budget so that one third of all nurses became contract hires with no work guarantees. The percentage of those leaving the profession surpassed 60%, and Head Nurse Chen now has no choice but to train a never-ending stream of new personnel. In addition to this, the management of nursing personnel in Taipei is not structurally unified. For example, nurses working in primary and middle schools come under the municipal Bureau of Education, and there is thus a great risk of creating holes in the epidemic prevention system. She proposes putting these nurses under the control of the municipal Bureau of Public Health to prevent a problem from arising.
Weng Lin-chung, superintendent of Taipei Municipal Chung Hsing Hospital, says after infections broke out in several hospitals, the number of outpatients quickly dropped by 50%. Obviously the 50% who did find it necessary to come to the hospital were patients who genuinely needed hospital care. This statistic highlights what is out of balance in Taiwan between the treatment system and the health centers which are charged with prevention. If health center nurses could get those patients who really don't need to visit the hospital to work on changing their diet and on personal hygiene, thus increasing their health consciousness, they wouldn't end up at the hospital in the first place, and the hospitals could concentrate all their efforts on the seriously ill.
Good health, not treatment
DPP Taipei City Councilor Hsu Chia-ching says the health center is the community's first line of defense against epidemics but that it is not tied in with the treatment structure. There is no professional intercourse between personnel. This is a major failing. Second, from the point of view of personnel and budget allocation, the current situation "favors doctors over nurses." The job of taking care of sick patients falls on the shoulders of the nurses yet they are not given adequate personnel resources. Finally, most of the budget goes to the treatment sector to buy equipment, expand hospitals and hire doctors. The recent 50% drop in outpatients at public hospitals shows that if half the outpatient budget were used for prevention the burden on the national budget could be reduced considerably. Hsu hopes Taipei Municipality can take the lead in reform and bring other cities and counties along with it.
Although the all-out "battle against the demon" has revealed a fundamental problem with Taiwan's public health system, this is also an opportunity to turn a crisis into a turning point.
Judged on capital efficiency, we can see the result of an over-reliance on treatment leads to a bottomless pit for expenses and an erosion of the national economy and personal finances. To replace this with something new, we should be thinking along the lines of encouraging good health and preventing disease as a substitute for the traditional diagnosis and treatment approach, because only by investing more capital in public health prevention measures can we lower significantly investment in the treatment sector. This is precisely the spirit behind the phrase "prevention is more important than treatment."

@List.jpg?w=522&h=410&mode=crop&format=webp&quality=80)





